Last year, Police Officer Louise, suffered a seizure and was rushed into hospital. Shocked, and caught up in a whirlwind of new information, Lou had little time to digest hearing the words “you have a reasonably sized brain tumour.” Her friends and family were soon by her side, and did everything they could to help.
In October, Lou’s partner got in touch with brainstrust to request a brain box. Months later, we heard from Lou who wanted to tell us just how much it meant to her, and her family, to receive the brain box when she did.
The brain box that my partner got for me from your charity really helped me throughout my journey. I recommend ordering it to anyone and it really does explain every stage in simple terms. It is great. I’ve got my stress ball brain still in my room, and I enjoyed using the face mask.
Lou was inspired by the support she received from charities like brainstrust, and has been fundraising ever since. With the overwhelming support and generosity of her family and friends, Lou has already raised an incredible £500 for a range of fantastic charities, and doesn’t plan to stop there.
Whilst on the road to recovery, Lou has taken the time to reflect on her journey so far. Below she shares a beautifully written, open and honest account of life with a brain tumour. We’re so grateful to receive Lou’s support, and honoured to share her inspirational story with you.
Lou’s Journey
I’m Lou, I am 31 years old, from Northamptonshire. I was diagnosed with a Grade 2 Astrocytoma last year at 30 years old. I was out for a run, around a lake in Milton Keynes, in June 2019 and had plans to visit my dad and other family later that day. I had never felt fitter and this is a picture of me I snapped around 5 minutes before my first fit.
It’s ok, I’m a police officer, I’ve probably overdone it running

I was nearing the end of my run when I suddenly felt very panicky. I felt like I urgently needed to change the time on my watch. I then started to spin around in circles. I was aware I was doing this but couldn’t stop myself. I saw people walking towards me, they must have thought I was acting very strange. I fell to the floor and that was the last thing I remembered.
I came back around and I was surrounded by unfamiliar people, looking down at me. I recall, a man asking me if he could phone anyone for me, they had already called an ambulance because, I learned, I had been shaking violently whilst I was unconscious. I could taste blood in my mouth and became aware that I had bitten my tongue. I felt very confused as to what had happened. I responded:
It’s ok, I’m a police officer, I’ve probably overdone it running.
I tried to get up, I wanted to try and walk it off, embarrassed at how I had created such a big scene. People told me to stay where I was, I heard sirens and two ambulances arrived shortly after. I was helped into one of the ambulances and asked very simple questions, for instance: my date of birth and where I lived. I couldn’t answer these questions at first, which was worrying, but the answers soon came back to me.
If it’s nothing, why can’t they tell me over the phone?
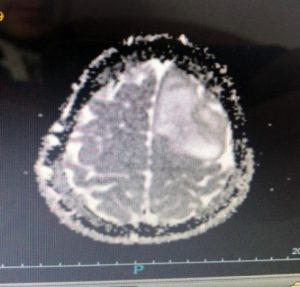 At Milton Keynes hospital I called my dad and my partner. Dad arrived quickly with one of my family and my partner left worked as soon as he could, as he was on duty. Initially everybody, including the nurses, thought I had probably overdone it with the run and this had caused the fit. I had no other symptoms. As a precaution, the doctor referred me for an MRI Scan. This was arranged for September 2019. Since I am highly claustrophobic, the thought of being placed into a small, noisy scanner, with a mental cage over my head was absolutely my worst nightmare. Still, I concluded, it had to be done, I wasn’t about to doubt medical advice. I must highlight and emphasis, that all of the NHS staff I encountered during my visit were absolutely brilliant, I cannot praise them enough.
At Milton Keynes hospital I called my dad and my partner. Dad arrived quickly with one of my family and my partner left worked as soon as he could, as he was on duty. Initially everybody, including the nurses, thought I had probably overdone it with the run and this had caused the fit. I had no other symptoms. As a precaution, the doctor referred me for an MRI Scan. This was arranged for September 2019. Since I am highly claustrophobic, the thought of being placed into a small, noisy scanner, with a mental cage over my head was absolutely my worst nightmare. Still, I concluded, it had to be done, I wasn’t about to doubt medical advice. I must highlight and emphasis, that all of the NHS staff I encountered during my visit were absolutely brilliant, I cannot praise them enough.
I will admit that I wasn’t concerned about the results and neither were my family or friends. So when I got a phone call the next day, asking for me to come to Milton Keynes hospital for my results, I remember saying to my partner and to my mum,
If it’s nothing, why can’t they tell me over the phone?
Not me? Surely not me?
I was really anxious about the phone call and about the apparent urgency. My partner and I attended together and I was told I had a ‘reasonable size’ brain tumour on my left frontal lobe.
This came as such a massive shock to me and if I’m honest I didn’t believe the consultant. You could argue that I was in denial but I thought he must have got me confused with someone else. Not me? Surely not me? I was extremely healthy, a fit, young female police officer, with my whole life ahead of me. I think it was worse that I had no other symptoms to refer to, nothing felt wrong with me.
My partner and I returned to where I had had my fit and to a pub there. I ordered their largest gin and tonic and tried to process what I’d just been told. I rang my mum whilst standing beside the lake and phoned my dad too. They couldn’t believe it either, nobody could believe it. The hospital advised me, I couldn’t drive anymore and I had to send my licence back to the DVLA. I continued to work, I hoped it might take my mind off it, but I had to be crewed with another officer, since I couldn’t drive. Work colleagues were just as shocked as I was.
My partner and I decided to move in together, to make getting around easier. We had only been together for about 9 months when I had my first fit. I honestly wouldn’t have blamed him if he thought this was all too much and walked away. Well, I would have blamed him a little bit but he didn’t and he has been and still is, my rock throughout all of this. He has been so incredibly supportive of me through this journey.
I was referred to Oxford hospital and I saw a surgeon who recommended that I had a biopsy undertaken on my tumour, to see what type it was and what grade. At the beginning of October 2019, I had a call whilst at work and was informed my biopsy would be the following day. I had no time to be nervous or scared, I just wanted to get it out the way and to find out what I was dealing with. So I could aim to get treated and to get on with my life.
How am I looking?
On the morning of my operation I was nervous. Thankfully, the surgeon, doctors and nurses came to see me to introduce themselves and put my mind at ease. I was wheeled downstairs, a large foil blanket was placed over me and filled with hot air. A mask was put over my mouth and the doctor asked me if I was meant to be working today. I don’t think I managed to answer the question. The gas took effect quickly and to can’t recall anything further.
I was woken up in a recovery room by a nurse, who was shouting my name. She wanted to know if I could hear her. She asked me how I was feeling and I replied saying:
How am I looking?
At the foremost in my mind, at that time, I was worried about the scar on top of my head and how much hair had been shaved. The nurse laughed and promised to get me a mirror shortly. I was set up with some considerable pain relief after my brain surgery. I surmised that I was ok, I could still talk, I had my memory and my sense of humour.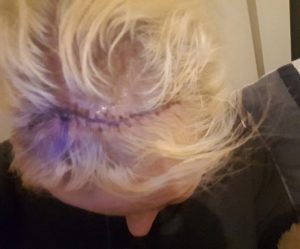
I was taken back to my room and I waited for my mum, my brother, my partner and his mum, to return. I had told them to go and get a drink and some lunch in Oxford, rather than waiting for me and worrying. That evening, my partner stood vigil by my bedside overnight, he also brought me a Macdonald’s, it tasted absolutely incredible. Everybody else came to see me the next morning. I was well rested, I had had no seizures (a possible side-effect of the biopsy), was going to the toilet on my own and I was eating ok. I was relieved to be allowed to go home.
I was put on long term sickness at work to recover. A few weeks later I was called back to Oxford for my results, my partner came with me. I was showed the scans and told I had a Grade 2 Astrocytoma brain tumour. It was benign and wasn’t cancerous but it needed treating to lower the chances of it turning cancerous. I asked if I was going to die and they couldn’t answer me. This scared me, it was a sobering response.
Am I going to die?
In October, a few weeks after my biopsy, I was in hospital for 10 days, this was due to a series of seizures that were caused by the biopsy. I remember waking up on the ward after being there for a few days and asking where I was and what was I doing here. This concerned the nurses and I was whisked off for an urgent CT scan. This scan showed I had a small bleed and swelling on the brain, again caused by the biopsy. The surgeon had taken a large sample of the tumour, to confirm it wasn’t cancerous.
I was put in my own room and kept in hospital. I was incredibly confused at the time, which again, was caused by the biopsy and the strong medication I was on. I genuinely thought I was going to die and that I had one night left to live. I messaged some close friends and family to say goodbye. I was having hallucinations and calling the nurses in every two minutes screaming and crying, pleading with them not to let me die. One sat and held my hand and promised I wasn’t going anywhere.
 Staff ended up putting an extra bed in my room, so that my partner and my mum could take turns to stay with me overnight. I remember feeling so afraid that I couldn’t look out the window, I thought I would see an ominous black figure waiting for me to notice them and that would be me dead. I remember my mum cuddling me to sleep, crying with me. She showing me a picture on her phone of a robin with a pink belly and it calmed me. It became a symbol of hope to me, seeing that picture meant that I was still here, still fighting for life. We still send the image to each other before saying goodnight to this day.
Staff ended up putting an extra bed in my room, so that my partner and my mum could take turns to stay with me overnight. I remember feeling so afraid that I couldn’t look out the window, I thought I would see an ominous black figure waiting for me to notice them and that would be me dead. I remember my mum cuddling me to sleep, crying with me. She showing me a picture on her phone of a robin with a pink belly and it calmed me. It became a symbol of hope to me, seeing that picture meant that I was still here, still fighting for life. We still send the image to each other before saying goodnight to this day.
One night, my partner stayed up with me all night. I was colouring in a picture of a peacock in an art book, because I couldn’t sleep. I was frightened I wouldn’t wake up again. This was by far my lowest point on the journey and even writing about it now makes me tearful. I have never been so scared in all my life. I was so scared and so sure I was going to die. I remember thinking, I wasn’t ready to miss out on the rest of my life. I have learned that this was one of worst nights for my family as well, especially when they couldn’t convince me that I would be ok. It took strong sleeping tablets for me find any rest that night. They knocked me out but meant I had had a good sleep. On waking up I felt much improved, I also felt relieved that I had not died. Once again the nurses were a credit to their profession, I must’ve been so frustrating and such a burden on them when I was ringing the bell every two minutes. They were so patient and kind, allowing my family stay to comfort me. I’ll never forget their care.
Eventually I was referred to the oncologist department at Northampton hospital where I was going to have my treatment. I met my doctor and nurse. I asked my doctor outright when I first met:
Am I going to die?
He looked at me and without hesitation he replied:
No, you will outlive me. You are not going anywhere. We are going to treat this and then you can get on with your life.
He said it so confidently that I burst into tears. I had not heard anything so re-assuring from any medical professionals up to that point. I was going to be ok and I would not die. The reply kept turning over and over in my mind. My tears made him well up as well and my partner too. He told me the best treatment for my type of tumour would be Radiotherapy. I needed to undergo scans, to have a radiotherapy mask made and 30 consecutive days of Radiotherapy.
This would shrink the tumour

My Radiotherapy was scheduled to start in November 2019 and finished in January 2020. This would shrink the tumour. I was also put on Dexamethasone steroids for my seizures in October and I am still on them now. These help to reduce the swelling on my brain, so I needed to take them during my Radiotherapy, because the tumour swells up before it gets smaller. I knew I needed Radiotherapy to treat my tumour but I was equally terrified of being pinned down by my face in a tight fitting mask designed to kept my head in the right position. I learned that the mask was a necessary evil so the treatment didn’t affect any of the good bits of my brain. Whilst it was a dreadful and unpleasant experience, I wouldn’t consider the alternative and the consequences of not undergoing the treatment.
The radiotherapists that gave me my treatment everyday were fantastic. I told them I was highly claustrophobic and would be confronting my fears. They were so very calm and patient with me. I went through the same routine each time treatment. The staff would start by trying to put the mask over my head, I’d freak out a bit but then and each time, I would have a word with myself. Eventually, I would allow them to put it on, but it took much self-control. Once it was on and the machine started, I told myself, each time, you are not stopping this machine. The staff would run out and get it off me as soon as possible.
I would talk to myself, in my head. I made myself promises that I would get a tattoo when I was better, that I would be back in the car soon, with a coffee and with my partner. He would always be waiting for me afterward with hot coffee. I came to associate the smell and the taste of that coffee with finishing my treatment and it helped. In honesty, I would often tell myself anything to get through it. I would say, I was strong, that I could do this. I kept my eyes closed the whole time. I did so until I heard them come running in, once it had finished. They took my mask off and lowered me down.
When I completed my treatment I rang the bell

As I became more used to the treatment it switched it around in my head. I told myself, my green mask was keeping me safe and that I should not be scared of it. I felt imagined the mask and I were working together to get rid of the tumour. Thanks to this, change in mind-set, treatments became much easier.
When I completed my treatment I rang the bell. I had everyone around me, which was such a special moment. I decided to take my mask home. With some help from a friend, I am planning to turn it into something special, a keepsake and a memory in defiance of the fact I faced my fears head on.
I lost my hair during radiotherapy. It fell out in clumps, so I had it shaved off by the hospital hairdresser. Seeing myself bald was a shock. It took a while to get used to. My face became really swollen during my radiotherapy, from the steroids and the radiotherapy. I also developed Cushing’s syndrome from being on the steroids for a long time. I struggled with this and to date, I am still now trying to get off the steroids. It retains water in your body, causing swelling. I have bad stretch marks all over my body, a hump on the back of my neck and a “moon” face. I had no energy and I was in a lot of pain. I was only just starting to get better. I was so knackered.
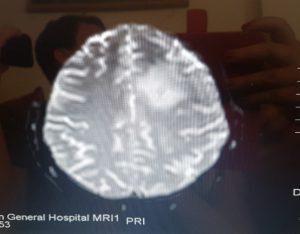
Each time the dosage of the steroids were reduced, I would have a seizure and be referred back to the ward by A+E. I was back in hospital in March 2020 because of this, for another 7 days. Once again I thought I was dying and would be seeing the ominous figure again. I was on a ward and I met some lovely ladies who were so patient with me, the doctors and nurses were too. The Corona Virus outbreak was just emerging, so my partner could only visit me for an hour a day. I remember telling him I was dying and he said do you really think I would be sat here so calmly if you were dying. That was a good point and I was able to accept his reasoning. I felt more at ease and was giving sleeping tablets again, had a good night sleep.
On waking up and I had not died, I was ok. My doctor confirmed I didn’t need any Chemotherapy, this was a relief, especially as I want children. My most recent scan showed that my tumour had reduced, it was a lot smaller and far less dense.
My journey isn’t over though
I am still trying to come off the steroids and this time my seizure medication has been increased so I am hoping, this time, it will work and I will be ok. This may mean I can get my body back, to get more energy and to start looking like me again. My hair is growing more with each passing day. My work have been amazing and supported me well. I am looking forward to going back, once I am fully recovered. I can’t wait to get my driving licence back, despite the jokes, I really am a good driver!
I feel very fortunate, in how things have turned out. I lost some friends along the way for reasons unknown to me, but I have also uncovered great friends, who I am much closer to now than before. Those I’ve found I can rely upon, to depend upon, when I needed them. I’ve made new friends too and I will keep them close. I have an amazing family, great work colleagues and my partner who is my best friend and soul mate. Without their support, I would have really struggled.
I still receive the odd letter or presents, at least once a week and I have done for a year now. This always cheers me up, knowing I have so much love and support. I completed a small step challenge, where I “walked” the equivalent distance to visit my family at their respective homes, during my daily walk. My nearest and dearest sponsored me and I raised money for brainstrust and the Brain Tumour Charity. When I have fully recovered and I have more energy, back I intend to raise more for them. My journey isn’t over though, I have another MRI scan coming up to see how my tumour is now. Hopefully it’s even smaller!

It hasn’t been easy, I lost my confidence and suffered from anxiety, which was hard. Everyone who knows me, knows me as a confident person, so reading this will surprise them. I have worked as a holiday rep, as cabin crew, in a prison, in a school and now the police. I have dealt with an awful lot in each these roles, but nothing prepared me for what I would have to endure on this journey. I feel I have a lot of life experience, for such a relatively young age but this has been hard. I truly believe, I can achieve anything if I put my mind to it and I have silenced my critics on that subject. I feel lucky, I didn’t lose my memory, or my speech, I am still able to write, to move and my personality has survived unscathed. I am still me. I really didn’t think anything like this would happen to me. I had no warning signs. The one seizure I had, I am grateful for because the tumour was found and it was treated, it was well treated. I was fit, healthy, happy and young and someday I hope to return to that lifestyle. So please enjoy your life because you never know what’s around the next corner.
Thank you so much for reading my story. I hope this is some help, to somebody. To those people who are going through what I have, keep going, keep believing.
Love Lou xx








