Becoming a caregiver for someone with a brain tumour can happen abruptly or creep in slowly unnoticed until one day you realise you are caring more for someone else than you are for yourself. Here you will find tips and information on how to look after yourself and create the space you need through this unexpected journey you find yourself on.
“Self-care is how you take your power back.”
Self care
As a caregiver, you may often feel like life is focused on your role of caring for someone with a brain tumour diagnosis. It may seem like there is no time to do things that you enjoy or you may feel like you don’t have any time to yourself.
Setting aside some time in your day to do something for yourself will give you some space from your caring role and bring some pleasure into your life.
Make yourself a list of things that you enjoy. Maybe these are things that you used to do regularly before the brain tumour diagnosis. These can be things that you can do alone or with your loved one as well.
Below are some of our suggestions to help get you started. Keep your list somewhere you can find it easily and try and tick off at least one a day.
Self care ideas to get you started
- Walk the dog
- Have a bath
- Watch a film
- Bake a cake
- Meet a friend
- Go out for dinner or get a takaway
- Organise a cupboard
- Read a book
- Plan a weekend away or a special day out
- Do an exercise class
- Treat yourself to something new
- Try some relaxation techniques
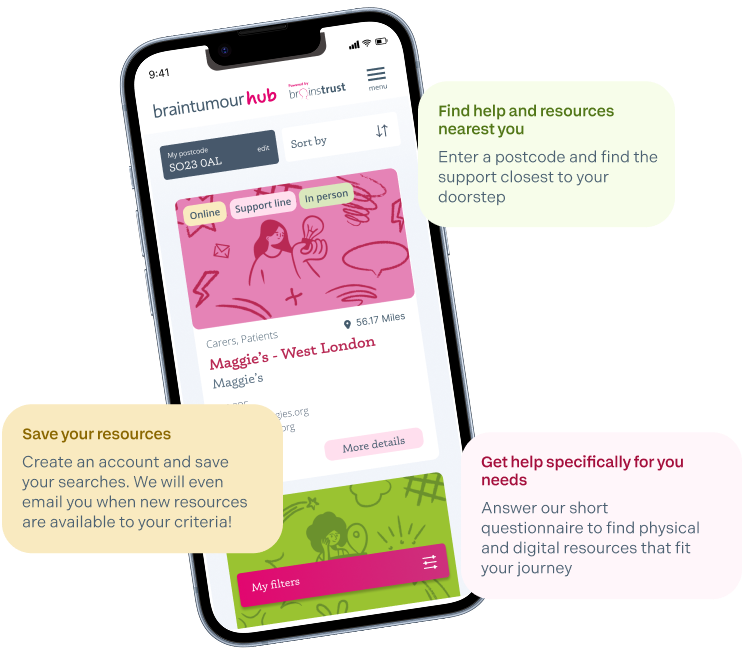
Created for brain tumour patients and caregivers, the brain tumour hub is an easy to navigate database of verified brain tumour support resources that have proven valuable to others.
Find support and resources from across the UK
Mindfulness
As a caregiver, you will have lots of different thoughts and emotions and may feel burdened and overwhelmed by these. By building mindfulness into a part of your day, this can help you feel more on top of things and in control.
Download mindfulness know how
Dealing with the overwhelm
When life suddenly changes and you find yourself in a caregiver role, it is hard to know which way to turn. Suddenly you are thrown into a new routine that you weren’t prepared for. In between hospital appointments, treatment, a new role in the household and caring for yourself you may find yourself feeling overwhelmed.
Download the Dealing with the overwhelm Know How
How to have a voice as a caregiver
Being a caregiver is a daunting role – you need compassion, fortitude and fierce resilience. And more often than not, you are living these values on behalf of your close person, but never for yourself.
Download the How to have a voice as a caregiver Know How
Living with uncertainty
When a loved one has been diagnosed with a brain tumour, you may feel that your life is less secure, more fragile than it once was. You find yourself living in a space where nothing seems anymore. It’s a scary place to be, and it can leave you feeling out of control and overwhelmed.
Download the How to live with uncertainty Know How
How to feel supported as a young caregiver
If you are under 18 years old and are helping to take care of someone with a brain tumour, you are a young caregiver. You could have a sibling, parent or relative with a brain tumour who you are helping to take care of.
Download the How to feel supported as a young caregiver Know How
How to prepare for medical appointments as a young caregiver
When someone you love is living with a brain tumour diagnosis, they will have regular medical appointments and check-ups at each stage of their pathway. These appointments are a key part of your loved one’s clinical care and are an opportunity for you to get key information and ask questions about their condition and treatment plan.
Download the How to prepare for medical appointments as a caregiver Know How
Did this information make you feel more resourced, more confident or more in control?
It has been a delight to collaborate with brainstrust. By referring our patients and their friends and family to this amazing charity we are able to ensure that all aspects of their needs are met.
Your help has been monumental to me in working through my thoughts and understanding of the disease. You have helped me gain a perspective on what has happened and to look at things in a new light. Thank you so very much for all your time and kindness.
Thank you for all your help, you were there when I was at my wits end and both the website and the box gave me the means to take back some control
Once again I can not tell you how reassured you made me feel yesterday. It was so important that I spoke to someone and you were there which I really appreciated
If it wasn't for brainstrust supporting me through my experience, I don't know where I would be right now
Your help has been monumental to me in working through my thoughts and understanding of the disease. You have helped me gain a perspective on what has happened and to look at things in a new light. Thank you so very much for all your time and kindness
Received the brain box yesterday. I cried with happiness. It's just what we needed - the booklets, information, tea and even hand cream. You have restored our faith in human nature