Debbie’s story
Debbie was still recovering from a traumatic illness in 2009 when she experienced further upheaval with a brain tumour diagnosis. Despite this, Debbie is now a Brainstrust peer supporter who is keen to share her extensive experience of living with a brain tumour, as outlined below.
After complaining of horrible post-headache sickness (like “a bad hangover”) and frequently falling over, in March 2012, Debbie’s GP shockingly told her about the tumour. This was followed by an appointment with a NHS consultant neurosurgeon, who believed the tumour was non-cancerous.
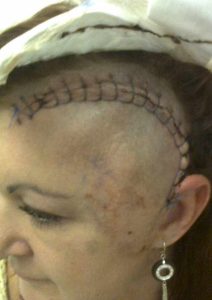 The hope of the initial surgery
The hope of the initial surgery
Just before her birthday, in July 2012, Debbie was hospitalized for 5 days after her first surgery. Debbie was left with a few reminders of the 10-hour operation like a skull indentation due to the introduced titanium mesh. However, she managed to return to work three months post- surgery.
The neurosurgeon thought the entire tumour, a meningioma, was removed. A meningioma originates in the layers of tissue that cover the brain and the spinal cord. According to Cancer Research UK, it is the most common type of benign tumour diagnosed in the UK.
The second op takes a greater toll
A long while after the initial surgery, Debbie started to feel unwell again. Unfortunately, as the tumour had grown again, she had to undergo a second operation, which took a greater toll on Debbie, so she had to give up work.
In this instance, the surgeon was certain that part of the tumour could not be touched without causing serious damage. Radiotherapy was considered but due to the positioning of the remaining tumour, there was a risk of leading to a neurodegenerative disease like Alzheimer’s.
The third surgery was the hardest
Unfortunately, her meningioma “is a bit of grower”, according to Debbie so she faced her third surgery in 2023. This time, the surgeon went in to remove sinuses and to compact the throat so the tumour didn’t grow into the stomach. Apart from feeling quite sick after the operation, it also resulted in cerebrospinal fluid in her middle ear drum.
Debbie is waiting for results due in April 2024 before yet another surgery to remove as much of the meningioma she named Bob the Builder, as he keeps her up all night and gives her headaches!
Debbie, the Peer Supporter
Debbie is usually quite independent and just “gets on with it”. However, she felt the need for support, particularly in between medical appointments, motivating her to become a peer supporter. Find out about our Peer Support service here. Involved in charitable work since her childhood days, Debbie enjoys being a supporter to other patients, lovingly nicknamed as her “brain buddies”. brainstrust support specialists put her in touch with patients struggling with different parts of their brain tumour journey.
As a good listener and a people person, the down-to-earth peer supporter is in touch with patients from Northern Ireland to Dubai. Despite living with the scars of battling her meningioma, Debbie still remains with a positive outlook: “Even if you have a tumour that you can’t get rid of… keep going, keep smiling!”
Other brainstrust support available to patients include face-to-face and online meetups with other sufferers. In fact, in the early days Brainstrust, Debbie found it useful to attend meetups to talk about her feelings and not to feel so alone. Recently, she attended brainstrust’s Meningioma Matters online meetup for the first time, after which a patient reached out to speak with her.









